- SELF STUDY MODULES
- 1. Intro to TBI
- 2. Communication
- 3. Skills for independence
- 4. Cognitive changes
- 5. Behaviour changes
- 6. Sexuality
- 7. Case management (BIR)
- 8. No longer available
- 9. Mobility & motor control
- 10. Mental health & TBI:
an introduction - 11. Mental health problems
and TBI: diagnosis
& management - 12. Working with Families
after Traumatic Injury:
An Introduction - 13. Goal setting
- 9.0 Aims
- 9.0A Take the PRE-Test
- 9.1 Brain injury and motor symptoms
- 9.2 Common physical presentations
- 9.3 Role of physiotherapy
- 9.4 Physiotherapy interventions
- 9.4a Motor retraining
- 9.4b Prevention of secondary complications
- 9.4c Fitness training
- 9.4d Regular physical activity
- 9.5 How can carers help make physiotherapy happen
- 9.6 Minimising risks
- 9.7 Take home messages
- 9.8 Resources
- 9.9 Take the POST-test
9.4b Physiotherapy interventions:
Prevention of Secondary Complications
As a result of weakness, changes in tone and muscle imbalances, some clients are at risk of developing muscle shortening and loss of joint mobility which can then lead to more permanent reduction in range and function. One of the primary goals of physiotherapy intervention is to identify muscle groups at risk of shortening and provide an appropriate intervention to maintain range.
Interventions may include the following:
- Low load prolonged stretches: target muscles are placed in a lengthened position by the use of splints or positioned using equipment such as soft weights to maintain the limb in that specific position.
Fig 1. (Above) An example of the use of bilateral knee extension splints and a hip abduction wedge.
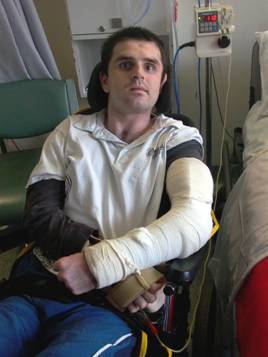
Fig 2. (above) Upper limb splints are commonly used to maintain elbow range of motion.
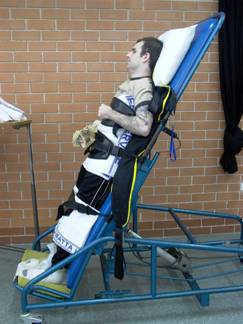
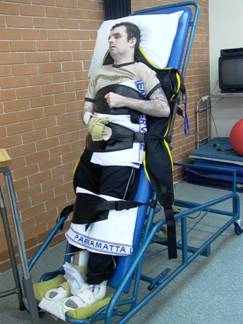
Fig 3 (a) and (b) (above) . Examples of an individual who has tilt tabling as part of his stretching programme
Tilt tabling: This can be done routinely in a physiotherapy programme to prevent shortening of the calf, knee and hip muscles; increase lung volumes; increase alertness and prevent loss of bone density in the lower limbs.
Positioning: Clients who are unable to move independently can spend long periods of time in the same position without a change in their posture. Trying to ensure clients are positioned so that there muscles are less likely to shorten is ideal. This may include positioning upper limbs on a wheelchair table so the shoulders rest in some external rotation, rather than resting across the client’s chest.
