- SELF STUDY MODULES
- 1. Intro to TBI
- 2. Communication
- 3. Skills for independence
- 4. Cognitive changes
- 5. Behaviour changes
- 6. Sexuality
- 7. Case management (BIR)
- 8. No longer available
- 9. Mobility & motor control
- 10. Mental health & TBI:
an introduction - 11. Mental health problems
and TBI: diagnosis
& management - 12. Working with Families
after Traumatic Injury:
An Introduction - 13. Goal setting
- 11.0 Aims
- 11.0A Take the PRE-Test
- 11.1 Mental health & mental illness & TBI
- 11.2 Factors affecting the risk of psychiatric illness after a TBI
- 11.3 The brain and psychiatric illness
- 11.4 Severity of a TBI
- 11.5 Types of mental health problems after a TBI
- a) Mood disorders
- b) Psychotic disorders
- c) Anxiety
- d) Personality
- 11.6 Sam : case study
- 11.7 Diagnostic challenges:
- a) Person with TBI
- b) Inherent in the disease
- c) Social environment
- d) Psychiatry and services
- 11.8 Management challenges
- a) Person with TBI
- b) Medical services
- c) Family
- d) Rehabilitation team
- 11.9 Take home messages
- 11.10 Resources
- 11.11 Take the POST-test
11.3 The brain and psychiatric illness
i) The Brain: video (4 min 10 secs)
This video provides a brief introduction to the brain, the different areas of the brain and mental illness.
The full text of the audio in the video is on the next tab.
The video may take a few moments to load. Click on the image to start the video.
ii) Video text
This is the text of the audio in the video.
The key determinant, of whether or not a person is at risk for psychiatric illness appears to be the location of the lesion at the time of the injury. Now while this can be very difficult to define in closed head injuries there are some generalisations we can make based on neuro-imaging and neuropsychological assessment.
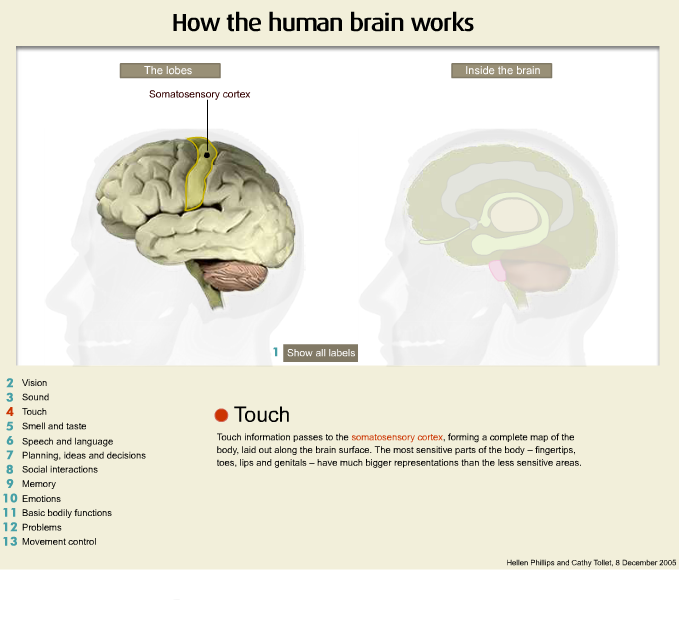
Throughout the modules I am going to be referring to various regions of the brain and I think this is a good opportunity for us to review the anatomy in a gross sense and to keep in mind where the various regions of the brain are when I refer to them throughout the entire modules. And what we are going to do is we are going to have a look at the model of the head with the brain exposed with part of the scalp and the skull removed.
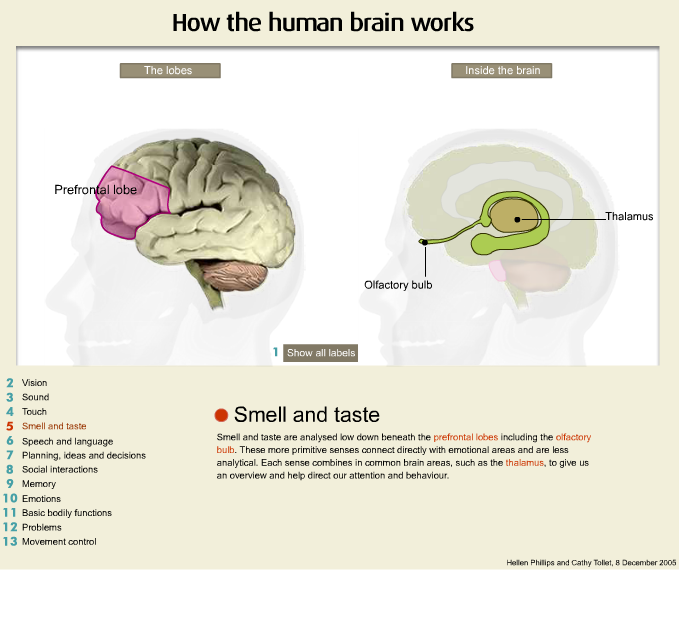
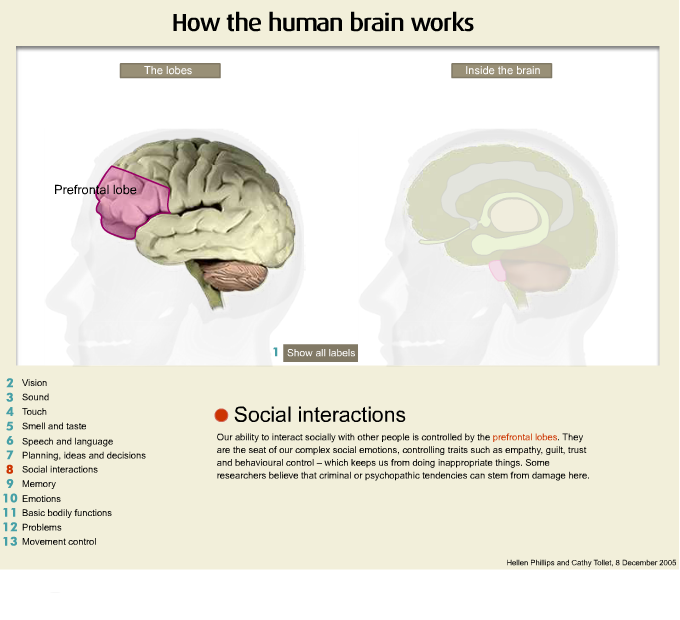
In particular, for the entire presentations we are going to be focusing on the frontal area of the brain. The frontal area is that area of the brain located above the bridge of the nose. The other very important area is that of the temporal area which is located above the ear.
I have here now a model of the brain which has been removed from the skull. In this model of the brain I am going to take away the cerebellum as this is not very important as far as psychiatric illness is concerned. The cerebellum is important for movement and procedural memory but it is not thought to have a big role as far as psychiatric disorder is concerned.
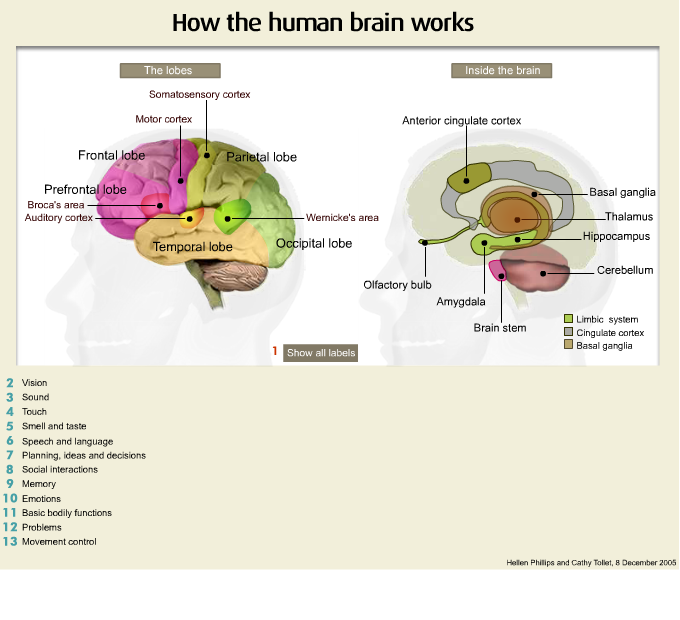
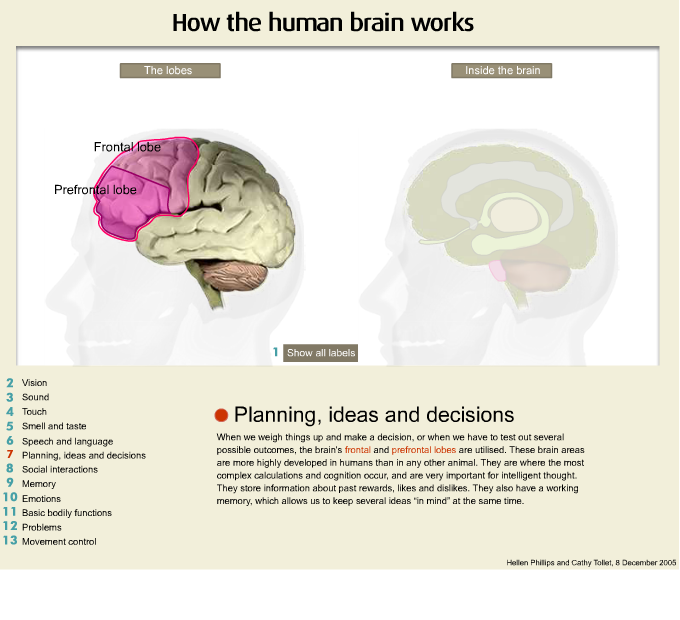
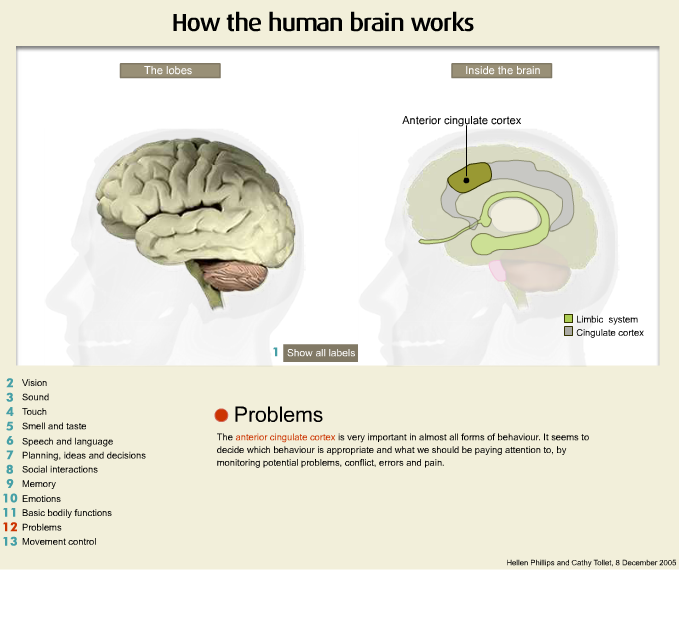
Now this is the top or the front part of the head and I am referring to the area of the frontal region and as you can see it is quite large and it is important for doing things such as planning, organising, problem solving and we often call the frontal lobes the chief executive of the brain because it is the chief executive of a company who is responsible for the running of the company and in many ways the frontal lobe of the brain is responsible for the running of the entire brain and our neurological functioning. So damage to the frontal regions of the brain frequently cause very substantial changes in behaviour and are significantly implicated in the onset of psychiatric illness.
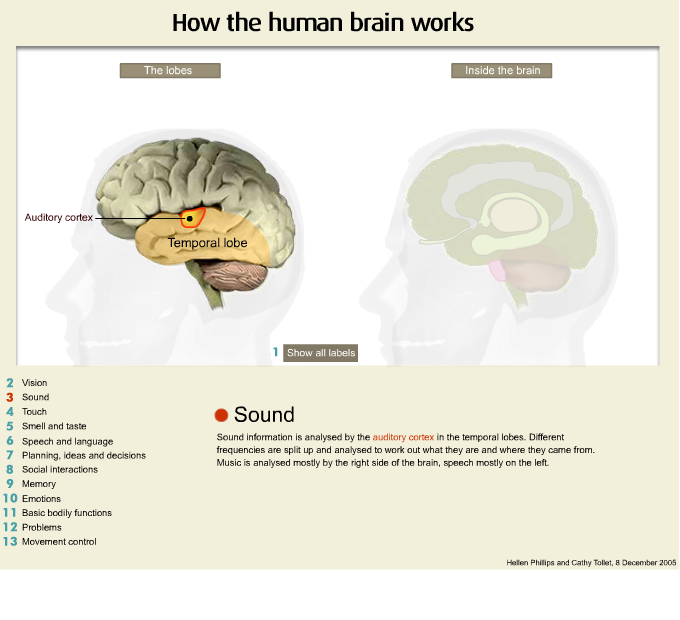
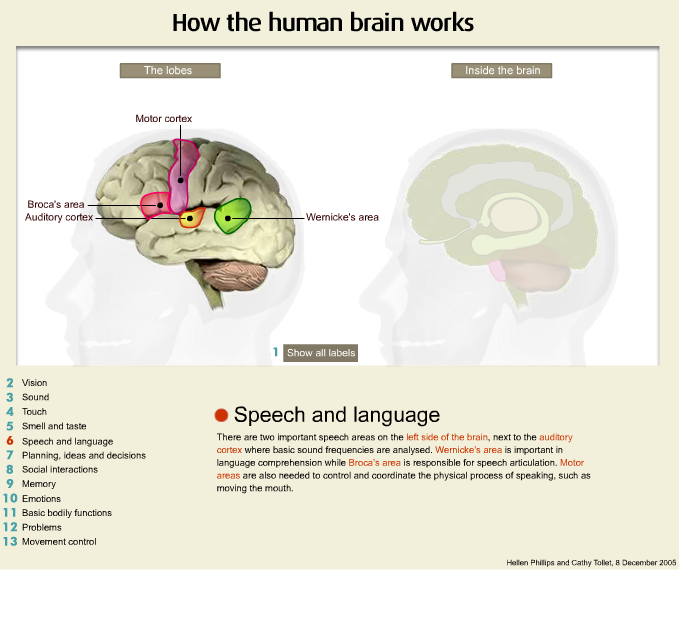
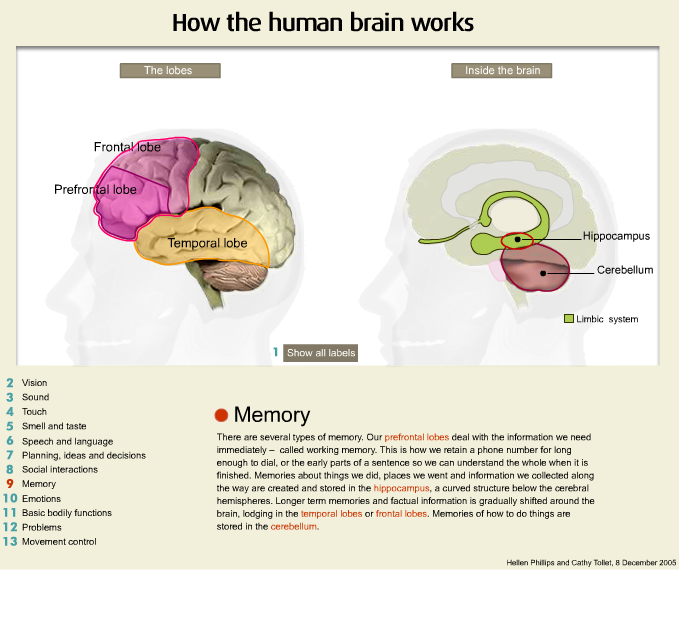
Another important area is the temporal area. I am just going to turn the model over and this is the temporal region here. Now the temporal regions of the brain are specialised according to the side of the brain. In people are right handed the left temporal area is very important for verbal memory and it is also important for the regulation and control of emotion. In right handed people the right temporal lobe is important for visual memory.
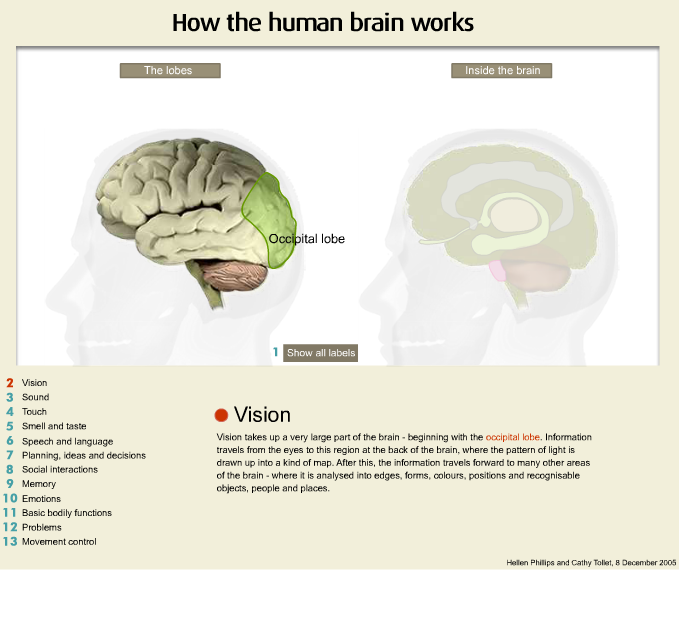
Another area of the brain that is very important is that of the parietal region and the parietal regions of the brain integrates information from all other areas of the brain. The parietal area frequently is implicated in the onset of delusional disorders so when you get damage in that area psychotic conditions frequently occur. At the rear part of the brain we have the occipital lobe which is very important for visual functioning.
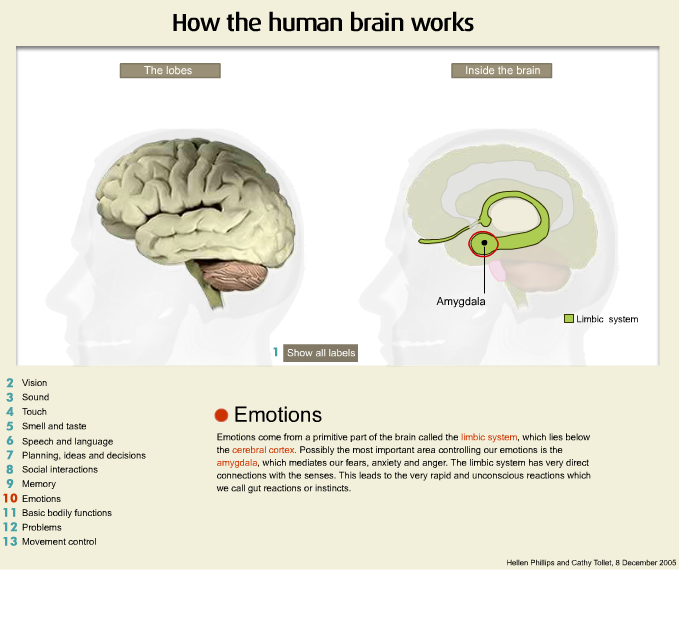
Now if we turn the brain over and have a look at the inside of the brain we have something called the corpus collosum, which is a series of fibres that connect, which are the connecting fibres of all the regions of the brain. If I remove the brain stem, and we are going to refer to that in a minute, I am now holding the temporal lobe of the brain and inside deep in the temporal lobe is part of the circuit of fibres that we call the limbic region or the limbic lobe and this is very important particularly for the regulation and control of the emotions.
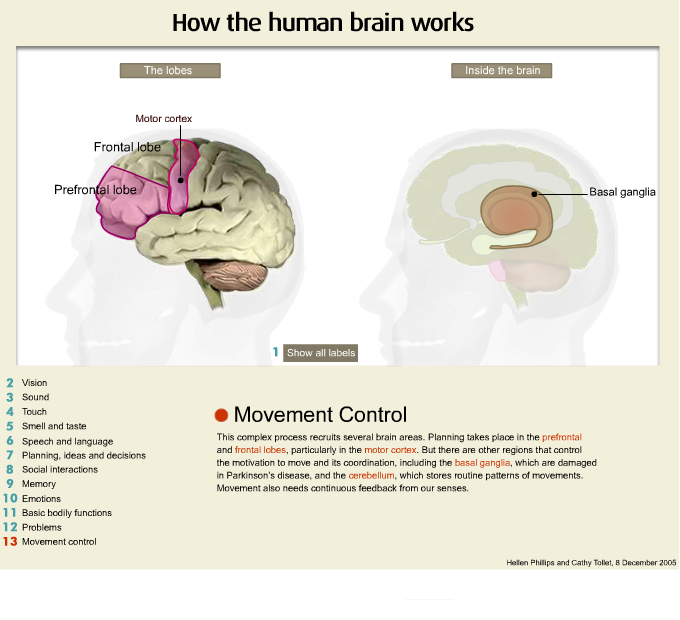
Lying underneath the cerebral cortices are the basal ganglia and these basal ganglia are a series of nuclei and nerve fibres that interconnect all areas of the brain. It is a very dense and compact area of the brain and if you have damage in this region, as can occur, particularly in high velocity injury, you often will have a very small area of damage but it has really widespread ramifications because the basal ganglia is so densely populated with important neuronal structures and it is the relay station, so damage here has effects throughout the entire cerebral cortex.
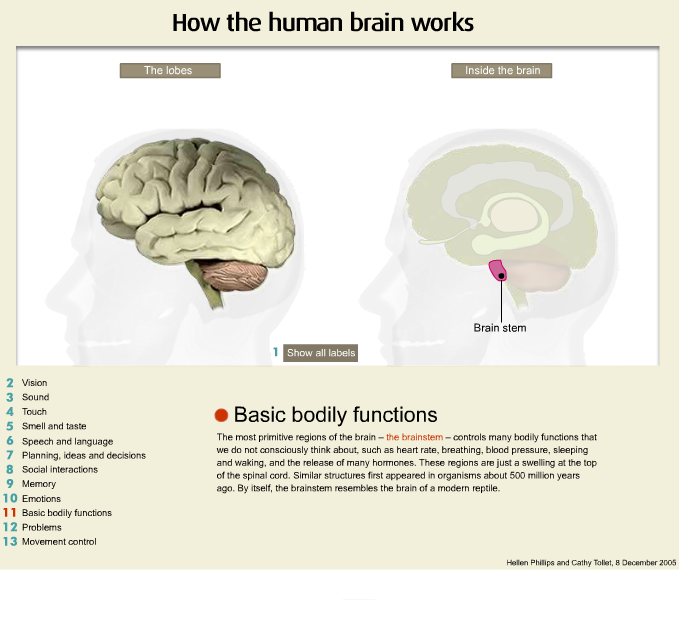
Below the basal ganglia we have the brain stem and the brain stem is very important as far as the general activation of the central nervous system and it is the site of origin of most areas of the brain for the important neuro-chemicals that are implicated in the various psychiatric illnesses. In particular, the area of the brain stem has projections to all parts of the brain, the serotonin, dopamine and acetylcholine which are the main neuro-chemicals that are implicated in the various psychiatric illnesses that we are going to be speaking about.
So we know that where the lesion occurs and the type of lesion is important and we also know that the severity of the lesion is extremely important. There appears to be a somewhat parabolic distribution of psychiatric illness when compared with the severity of brain injury. For people with the moderate to severe brain injuries there is quite a high incidence of psychiatric illness when compared to the normal population. There is less significant psychiatric illness for the mild traumatic brain injuries although people with mild traumatic brain injury can have a lot of dysfunction, the type of psychiatric illness is usually less severe. And of course, at the very severe end of the spectrum of traumatic brain injury often the person's degree of dysfunction of neurological capacity, their ability to speak and communicate is so profoundly impaired that we are unable to make an assessment of whether or not they have a psychiatric illness .
The fact that there is less psychiatric illness in the extremely severe brain injured people may be more an issue of our inability to assess than a reality .
SLIDES:
To pause: Hover mouse over slide. To continue: move mouse off slide.
To go to a specific slide: Click on slide numbers below.
Answer these questions:
Is the location of the brain injury a key determinant for the risk of psychiatric illness after a brain injury?
Which of the following areas of the brain are particularly important in relation to psychiatric illness after a brain injury?
Cerebellum, frontal region, parietal region, basal ganglia.
Who is most at risk of diagnosed metal illness after a TBI? People with mild, moderate or severe TBIs?